Care Program
A Care Program in Salesforce Health Cloud is an enrolment-based program that patients participate in over time: a Diabetes Management Program, a Mental Health Coaching Cohort, a Post-Discharge Follow-Up Program, a Maternity Support Program.
Definition
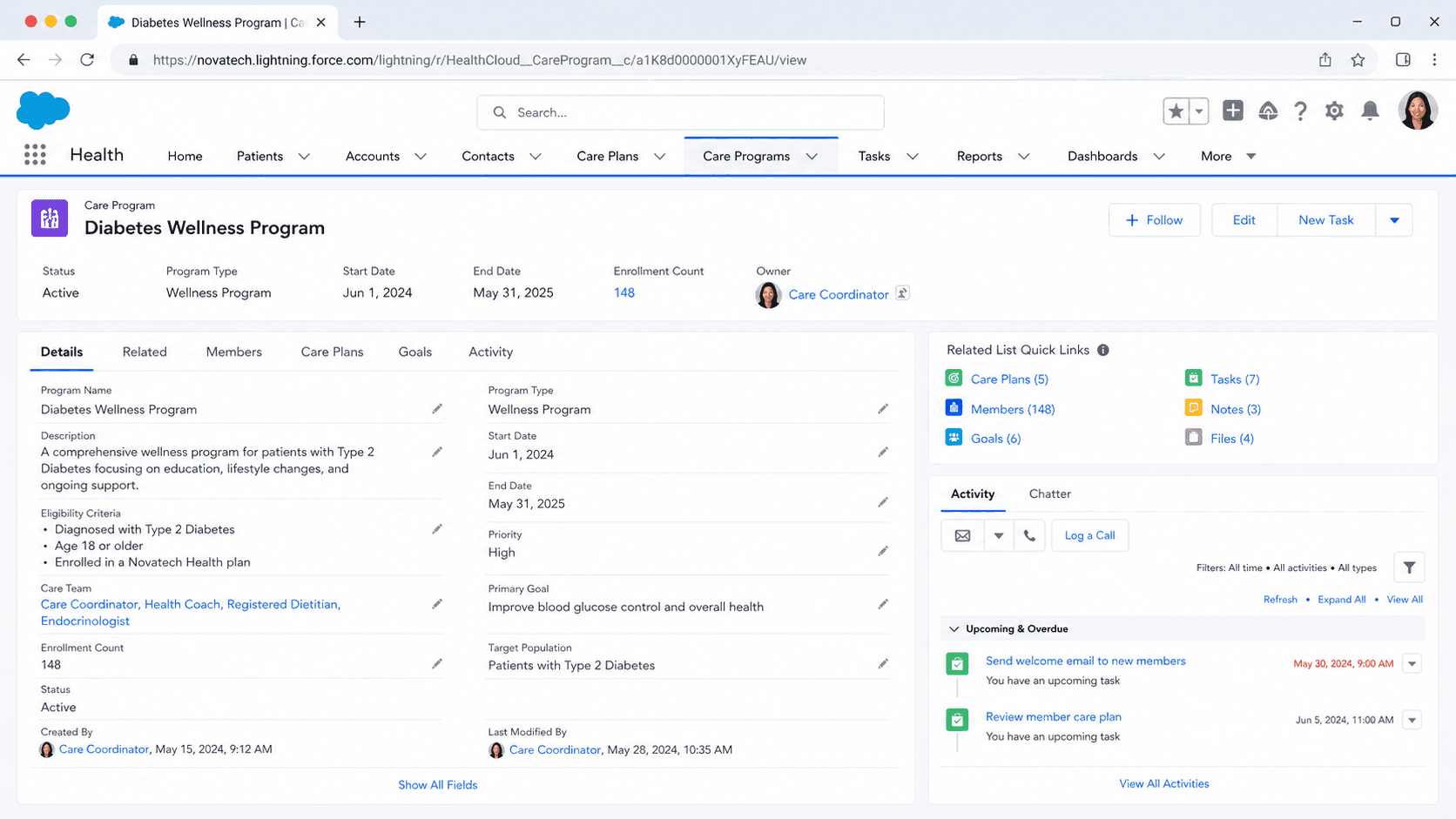
A Care Program in Salesforce Health Cloud is an enrolment-based program that patients participate in over time: a Diabetes Management Program, a Mental Health Coaching Cohort, a Post-Discharge Follow-Up Program, a Maternity Support Program. The Care Program record defines the program's name, sponsor, eligibility criteria, target outcomes, and budget. Patients enrol into a Care Program through a Care Program Enrollee record, which tracks their participation status, start date, end date, assigned Care Coordinator, and progress milestones. A single Care Program serves many enrollees; one patient can be enrolled in multiple Care Programs simultaneously.
Care Programs are the macro-level structure that Care Plans sit inside. Where a Care Plan organises work around one patient, a Care Program organises a population of patients pursuing a shared goal (managing diabetes, recovering from surgery, navigating maternity). Health plans, providers, and disease-management vendors use Care Programs to run population health programs at scale. The Care Program record carries the budget, the staffing model, the reporting framework, and the outcomes metrics that justify the program to leadership. Enrollees inherit the program's standard Care Plan Template, get assigned Care Team members from the program's pool, and roll up into program-level outcomes reports.
How Care Programs structure population health at scale
The Care Program data model
Care Program is the parent record, with child Care Program Enrollees (one per enrolled patient). Each Enrollee links back to the Care Program plus the Patient (Person Account). The Care Program also owns associated Care Plan Templates, default Care Team roles, eligibility criteria, and budget.
Enrolment and eligibility
Patients enrol through an explicit Care Program Enrollment process. Health Cloud supports eligibility criteria (clinical markers, demographic filters, insurance coverage) that auto-suggest or auto-enrol qualifying patients. Manual enrolment supports cases where clinical judgement overrides automated rules.
Care Plans inside a Care Program
Each Enrollee typically gets a Care Plan instantiated from the Care Program's standard template. The Care Plan handles the individual patient's Goals, Problems, and Tasks; the Care Program provides the standardised structure across enrollees.
Care Team assignment
Care Programs maintain a pool of Care Team members (Care Coordinators, social workers, RN coaches). New enrollees get assigned from this pool based on caseload, language, geography, or specialty. Mature Care Programs balance caseloads explicitly to prevent any one coordinator from overload.
Outcomes reporting
Care Programs roll up enrollee-level outcomes (Goal completion, readmission rates, condition stabilisation) into program-level dashboards. Reporting is how programs prove ROI and adjust scope. Without aggregate outcomes reporting, Care Programs cannot defend themselves at budget cycles.
Public Sector Programs equivalent
Salesforce Public Sector Solutions uses similar structure under different vocabulary: Benefits Programs, Case Programs, Participants. The data model parallels Care Programs in Health Cloud. Government social-services agencies build the same kind of enrolment-based population management on this stack.
Integration with claims, EHRs, and CRM
Production Care Programs integrate with external systems: claims data to identify eligible patients, EHRs to import clinical history, billing systems for program-funded services. The integration usually flows through MuleSoft or Data Cloud. Without integration, Care Programs accumulate manual data entry that does not scale.
Common operational pitfalls
Three patterns recur. Eligibility criteria too loose enrolls patients who do not benefit. Too tight misses patients who would. Caseload imbalance burns out Care Coordinators. And missing outcomes reporting means the program cannot prove value when budget reviews arrive. Each is addressable with deliberate program design and routine review.
How to design a Care Program
Care Programs are designed by clinical leadership, configured by Health Cloud admins, and operated by Care Coordinators. The configuration steps below assume the program design is settled.
- Create the Care Program record
From the Care Programs tab, click New. Provide Name, Sponsor, Description, Start Date, End Date, Budget, and Eligibility Criteria.
- Attach a Care Plan Template
Link the Care Program to the relevant Care Plan Template that will be applied to each Enrollee on enrolment.
- Define Care Team pool and assignment rules
Identify which Care Coordinators are part of this program's pool. Configure assignment logic (round-robin, language match, specialty match).
- Configure enrolment workflows
Set up automation that enrolls eligible patients, including the manual approval step where required. Map external data (claims, EHR) into the eligibility criteria.
- Build outcomes dashboards
Create reports and dashboards on enrollee outcomes (Goal completion, condition stabilisation, readmissions). Schedule monthly leadership reviews.
The standard object representing the program.
The per-patient enrolment record.
Standard plan applied to each Enrollee.
Rules for which patients qualify.
Reporting surface that justifies the program at review cycles.
- Eligibility criteria too loose dilute outcomes; too tight miss the patients who would benefit. Tune carefully.
- Caseload imbalance burns out Care Coordinators. Build assignment logic that balances explicitly.
- Outcomes reporting takes months to accumulate signal. Plan for early proxy metrics until real outcomes data lands.
- Integration with claims, EHR, and billing is essential at scale. Without it, manual data entry kills the operational model.
Trust & references
Cross-checked against the following references.
- Care Programs in Health CloudSalesforce Help
- Health Cloud OverviewSalesforce Help
Straight from the source - Salesforce's reference material on Care Program.
- Care Program EnrollmentSalesforce Help
About the Author
Dipojjal Chakrabarti is a B2C Solution Architect with 29 Salesforce certifications and over 13 years in the Salesforce ecosystem. He runs salesforcedictionary.com to help admins, developers, architects, and cert/interview candidates sharpen their fundamentals. More about Dipojjal.
Test your knowledge
Q1. What is a Care Program?
Q2. How does a patient become part of a Care Program?
Q3. How do Care Programs and Care Plans work together?
Discussion
Loading discussion…